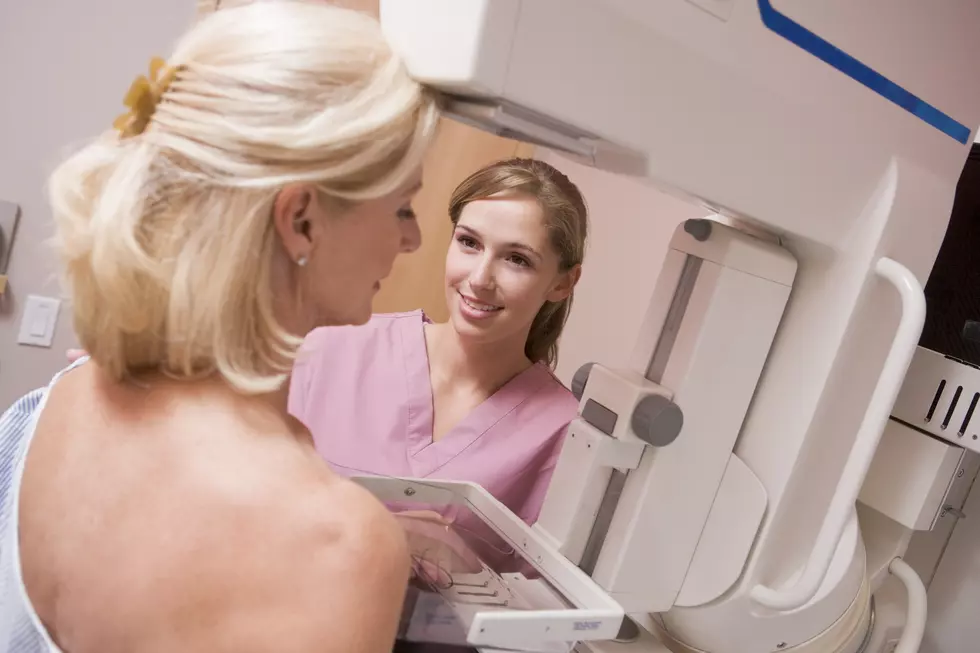
Simply talking to your doctor can go a long way in surviving breast cancer
Female breast cancer is the most commonly diagnosed cancer worldwide, according to The American Cancer Society.
What are some other important statistics?
There have been 8,410 new cases of female breast cancer in 2022 in New Jersey and 1,210 deaths according to their statistics.
Nationally, ACS estimated nearly 300,000 women will be diagnosed this year. It’s the second most common cause of cancer in women, second to skin cancer.
About 2,700 men across the country are estimated to be diagnosed with breast cancer in 2022.
But thanks to early detection and improved treatment, the number of women dying from the disease declined by 42 percent over three decades.
The number of breast cancer cases has been going up year after year, but that’s actually good news, said Dr. Arif Kamal, Chief Patient Officer at The American Cancer Society.
“We’re catching more cancers and we’re catching them earlier and that’s important because the earlier we catch cancer, the more likely we are to cure it,” Kamal said.
For example, if the cancer is still small and in the breast itself, then the chance of cure is 90 percent or higher.
But, once it’s caught later, meaning it’s had time to metastasize and spread, the chances of curing it goes down significantly and quickly, he said.
What is the current advice regarding mammograms?
Kamal said first and foremost, both men and women must have a conversation with their doctors about their risk of breast cancer either today or in the future.
That risk assessment starts with being clear and concise about a patient’s family history.
Kamal said a patient’s uncle may have had colorectal cancer or an aunt had uterine cancer or their mom had ovarian cancer. None of those diagnoses are breast cancer, but he said they are linked to breast cancer, and actually increase the risk of breast cancer to the patient, who could very well only be in their 20s or 30s, he added.
So, understanding that family history and sharing that history with a clinician is what needs to happen first, Kamal said.
Once that conversation happens, doctors then have a better idea of a patient’s risk. It could be an average risk or an increased risk.
What is an increased risk of getting breast cancer mean?
For increased risk, doctors may start mammograms, MRIs, and annual physicals at an earlier age, say in a patient’s 20s or 30s, based on that risk, he said.
What is average risk?
For average-risk women, Kamal said they should start mammograms or think about mammograms at age 40. Then, at age 45 and onwards, get a mammogram every year, with the option of getting them every two years after the age of 55.
Recognizing that a person is at average risk or at increased risk of getting breast cancer starts with a conversation with the patient’s doctor, Kamal reiterated.
What about breast cancer screenings?
Recent research from ACS showed breast cancer screening dropped 6 percent due to the COVID-19 pandemic.
This is both good and bad news, Kamal said. The bad news is that about two million women missed a routine and recommended mammogram during the pandemic, mainly because the doctor asked them to stay away from medical settings.
But, the good news is that doctors have not missed the window of opportunity to catch up and prevent an uptick in more dangerous and deadly breast cancer diagnoses down the road, he said.
“What I mean by that is that breast cancer generally takes years to grow. Not months, not days, not weeks, but years, which means that if a person missed a screening or mammogram in the last two years, then making up for that in the next year, really making now and 2023 the time to catch up on that, means we are not losing anything over the last two years,” Kamal said.
What about conducting self-breast exams?
Talk to your doctor to see if a self-breast exam is even the right approach, said Kamal.
“I say that because what we don’t want is any unnecessary loss of sleep,” he said. It’s possible a person may feel something on a Friday night, then they worry all weekend long it’s something ominous.
An individualized approach means a man or woman talks to the doctor to find out what they’re feeling and what is normal for them to find.
Kamal said there are women with breasts who have things they can feel in there because of several factors including, the architecture of their breasts, where they are in their cycle, whether they are pre or post-menopausal, and cystic changes which can be benign.
Some women have dense breasts, he said. With density, they will most likely feel something in their breast. Mammography may not even be the right way to find an abnormality.
“Understanding what I would be looking for in feeling and what would truly be different is an important conversation to have with your doctor and it’s a very individualized one,” Kamal said.
Once a patient knows what to look for, then the threshold to know when to call or when to worry about something is a lot clearer.
Most guidelines, including those from ACS, don’t advocate for self-breast exams for every person at all times, regardless of risk.
Have that conversation with the doctor, understand how to do it well, understand how to do the self-breast exam well, and know when to call, when to worry about something, and move forward.
Can men get breast cancer?
Yes. Kamal says it’s not common but breast cancer among men should be recognized. Generally speaking, he said breast cancer in men is driven by hormones in that person’s body and can be addressed with typical treatments.
But men with a family history of ovarian, uterine, endometrial, gastro, and colorectal cancers, are at a higher risk of getting breast cancer, and that cancer can sneak up on them, Kamal said.
He said men need to pay close attention to their breast tissue and pay attention to their family history.
What is the takeaway?
“What I would say is, this starts at the beginning with a conversation with your doctor to say, what should I be thinking about, what should I be looking for, what are the right tests, when should I get started, and by the way, here is my family history, so does this change our approach,”? Kamal summed up.
Jen Ursillo is a reporter and anchor for New Jersey 101.5. You can reach her at jennifer.ursillo@townsquaremedia.com
Click here to contact an editor about feedback or a correction for this story.
11 years later — Sandy makes landfall in New Jersey
More From 92.7 WOBM










